An RPM solution that works for you
Discover the benefits of our comprehensive, AI-powered remote patient monitoring system and how it can help your healthcare organization.
Get all the support you need to make remote patient monitoring programs truly successful. Our people, software, and devices help keep you focused on what matters – healthy patients, compliant programs, and meaningful revenue.
Remote patient monitoring (RPM) encourages patients to take control of their current health while delivering vital information to clinicians between office visits. A single enrolled Medicare patient can conservatively generate $47 per month in practice revenue, all improving their health outcomes and increasing patient care plan compliance.
Are you new to RPM? Do you have a program needing a boost? We guide you through the ever-changing regulatory and billing requirements so you can remain focused on your patients.
Discover the benefits of our comprehensive, AI-powered remote patient monitoring system and how it can help your healthcare organization.
Device data feeds into each patient’s profile where healthcare providers can easily monitor patient vitals and customize graphs that chart progress over time.
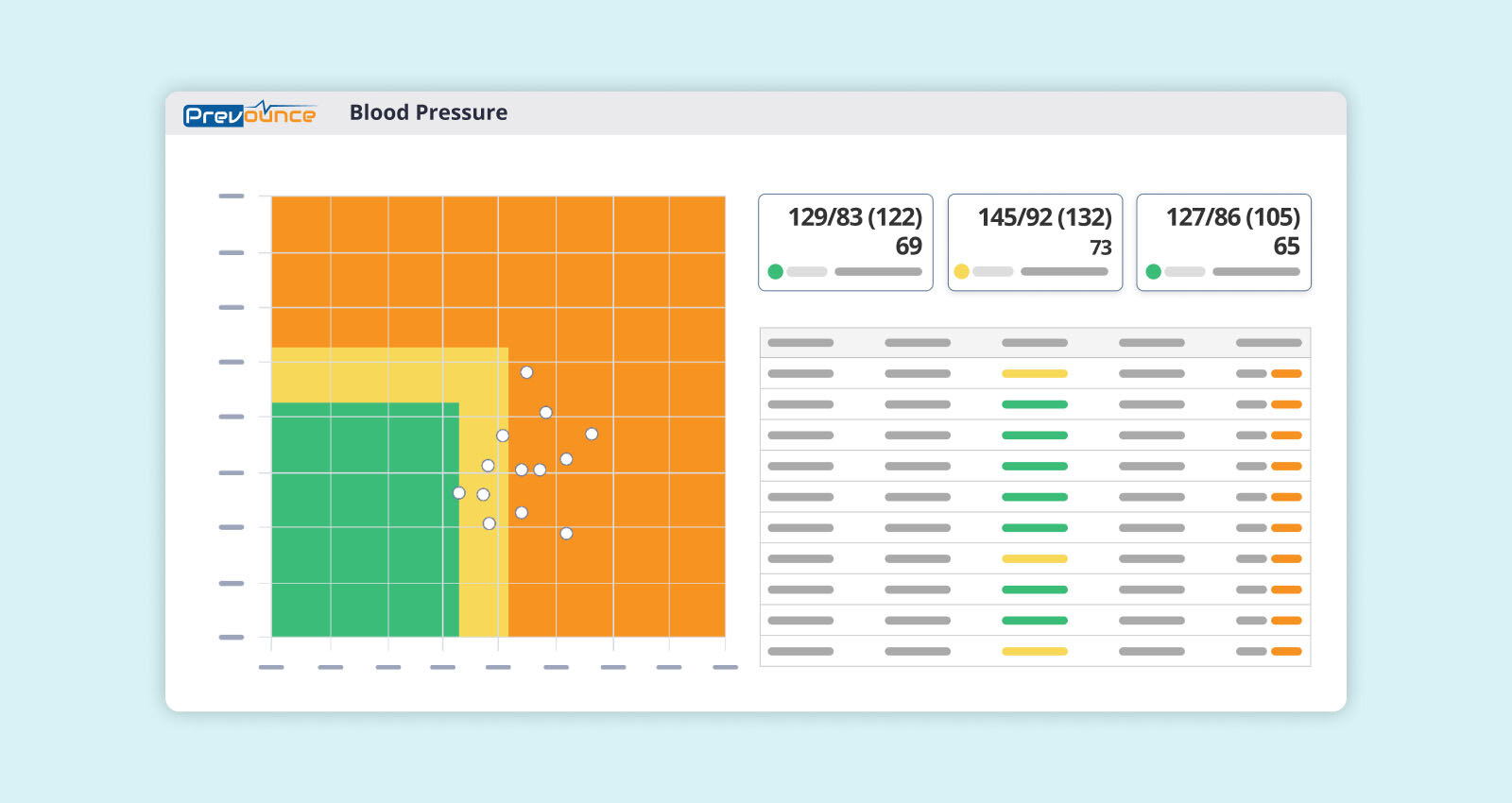
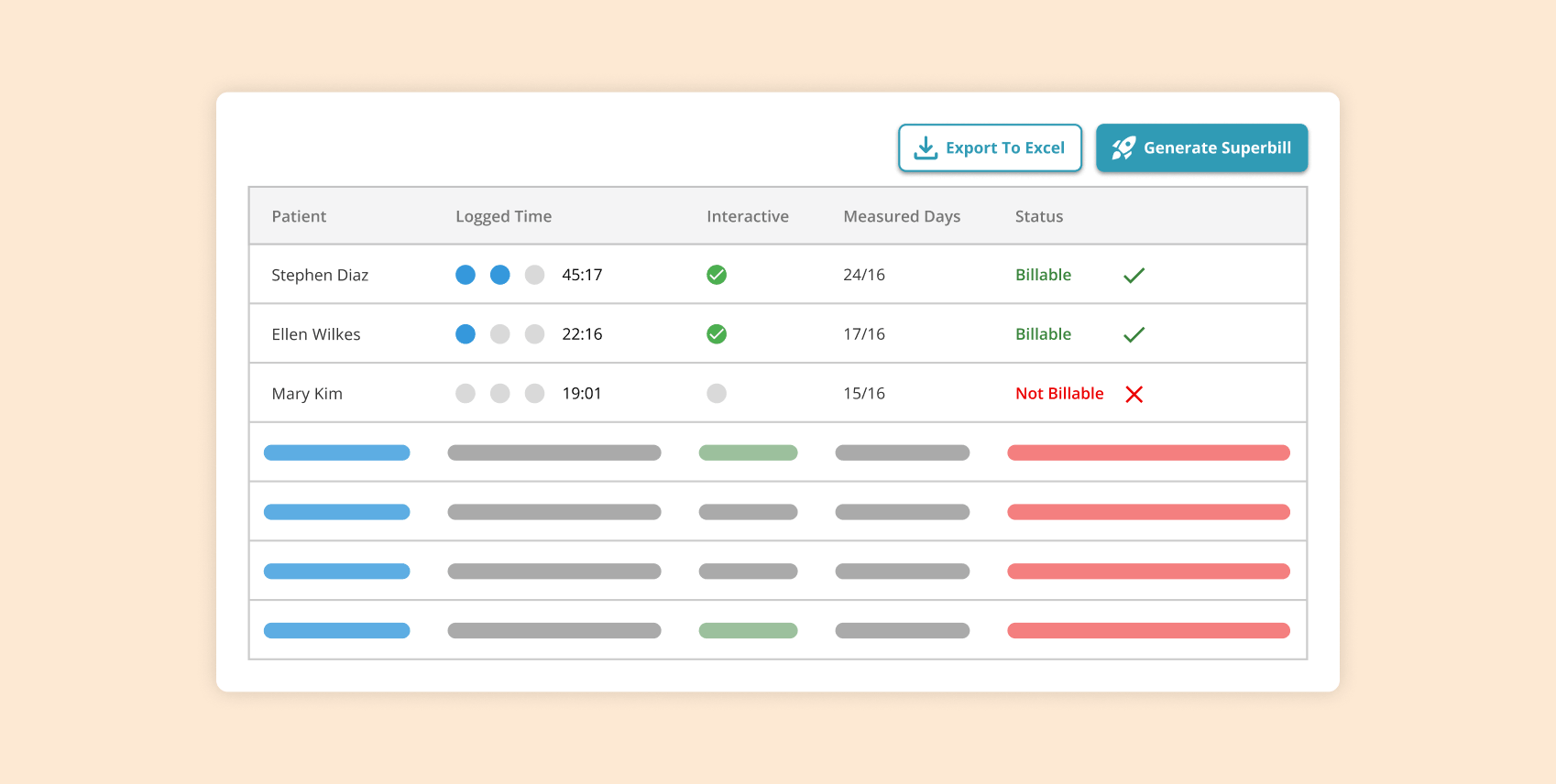
Staff can view patient compliance toward monthly billing requirements and seamlessly capture time spent on care management activities.
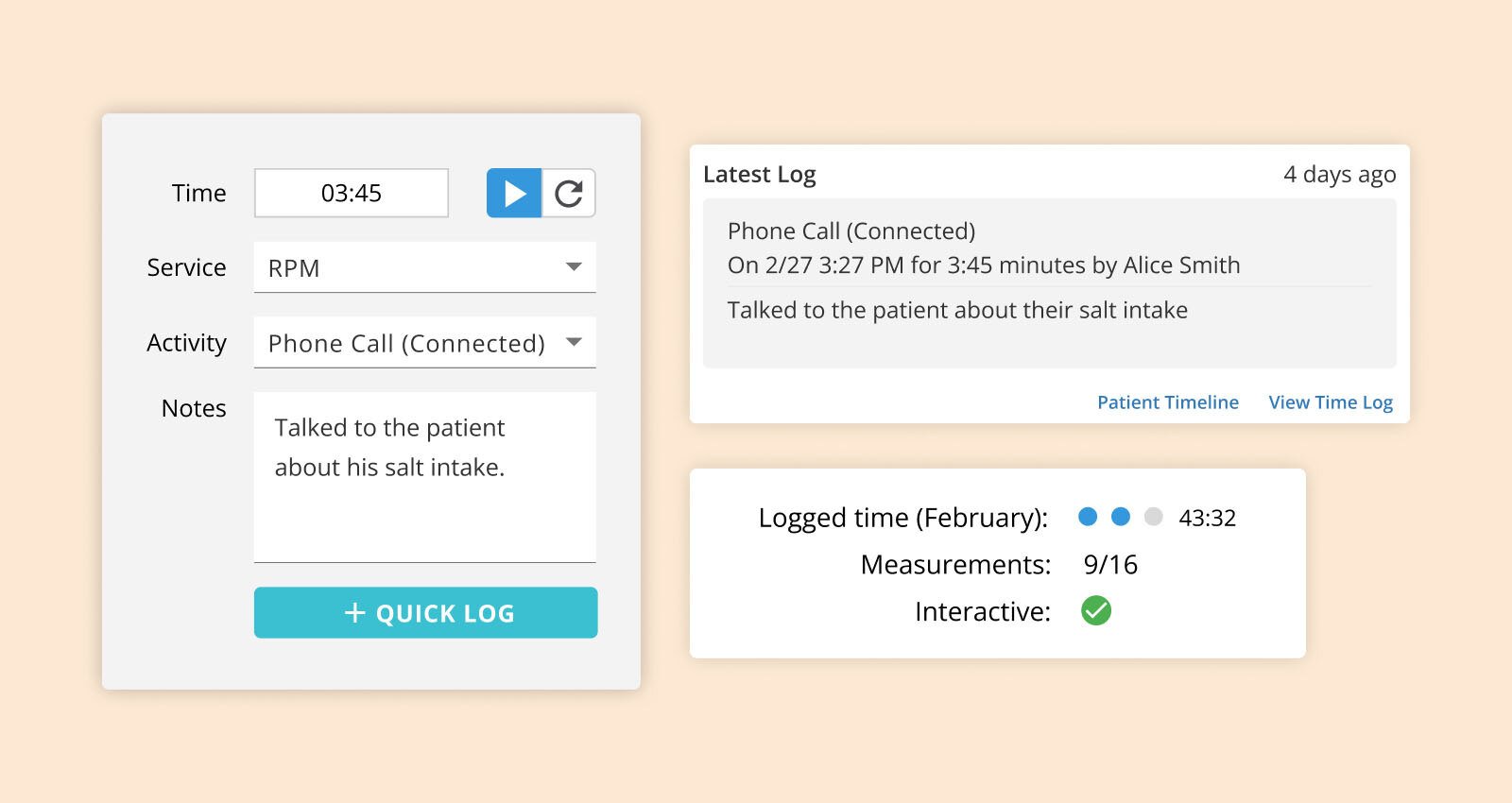
Quickly identify trends or emerging health concerns with the help of clinically-trained generative AI. Embedded AI tools analyze historical RPM device readings and care notes to deliver actionable care summaries and recommendations

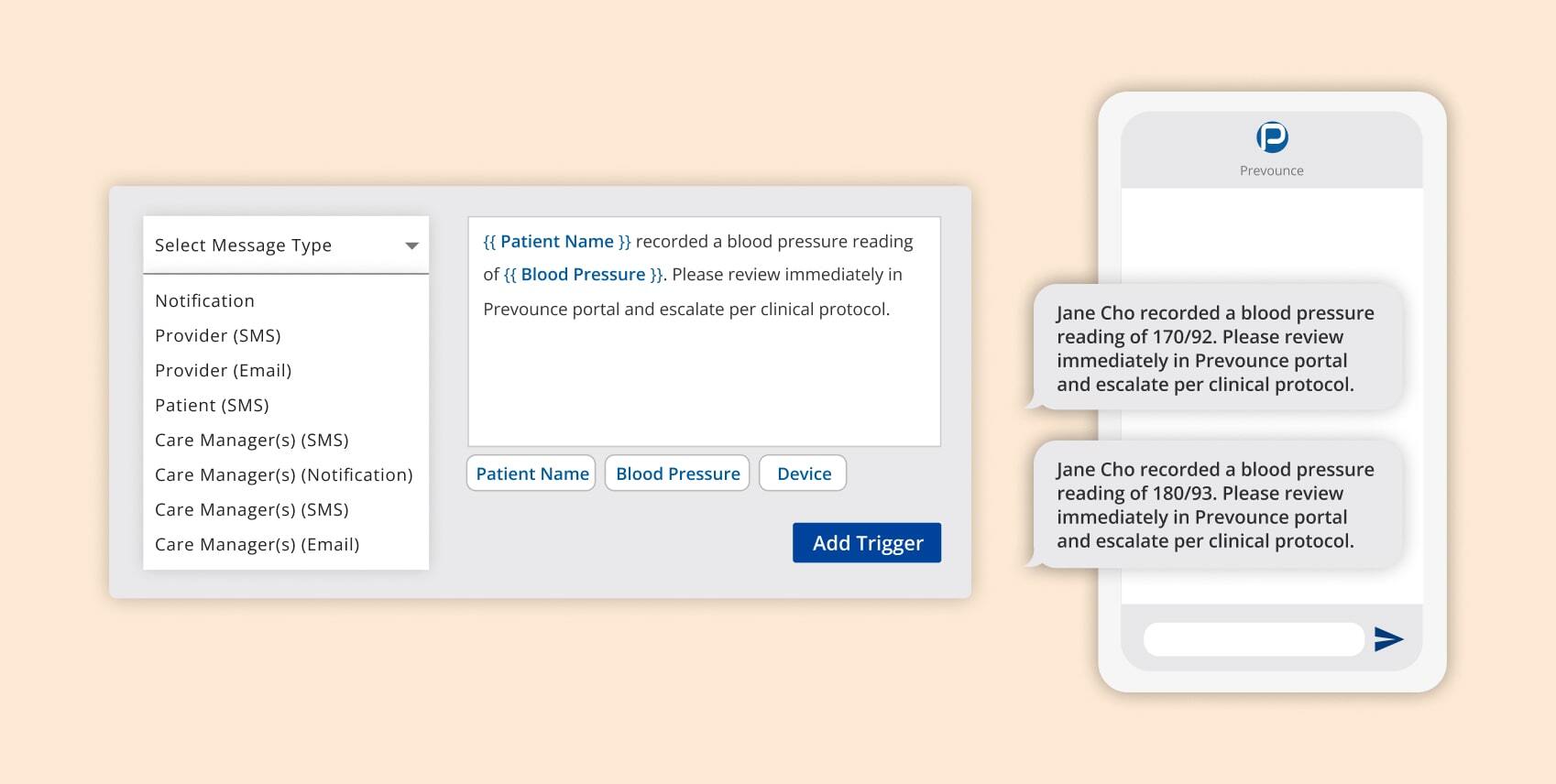
Set up customizable, automated email or text reminders to patients and alerts to healthcare providers when readings fall outside of normal ranges.
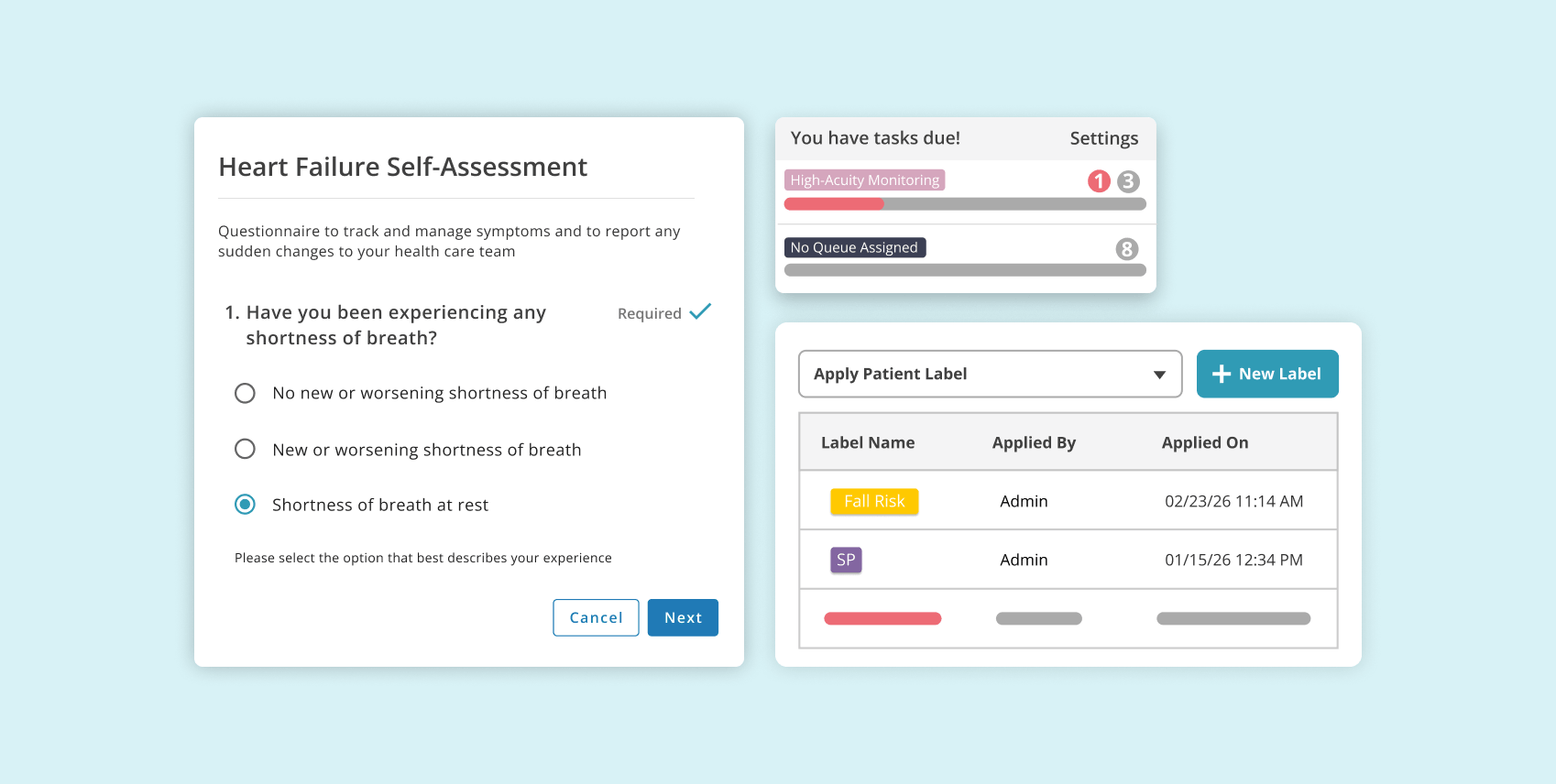
Capture patient-reported outcomes through easily deployable questionnaires, categorize patient populations with custom labels, and prioritize care manager activities with individual and team-based tasking.
Our platform generates a suggested superbill every month clearly showing all billable RPM codes for each patient for easy coding and billing.
All patient data is stored securely, end-to-end, from collection on the patient’s device to storage on our HIPAA- and HITRUST-compliant platform.
.jpg)
Patients participating in remote patient monitoring programs are more engaged in their health and experience improved condition management and outcomes.
Tailor the patient experience. Customize our cellular-connected, clinically validated devices and kits with your branding, printed inserts, patient education assets, and more.

Whether you are looking for easy access to patient readings or a comprehensive device management platform, our Pylo API is the easiest way to integrate cellular (LTE) remote patient monitoring into any patient health application or management system.
RPM benefits patients supported by a variety of specialists. Our solutions help ensure specialists have what they need to support their patients. We cover a range of specialties on a single platform for administrative efficiency, without compromising on individual clinician needs.
Reduce patient risk and mortality, improve care between visits, and grow your practice.
Adjust medications, advise on lifestyle changes, and increase patient volume and satisfaction.
Help patients make lifestyle and behavior changes necessary for weight loss and management.
Execute long-term care plans, grow patient volume, and protect reimbursements.
Enhance patient care in maternal health by using remote monitoring to track vital metrics.
Systematically improve management of the most prevalent and dangerous disease states.
Patients with at least two chronic conditions can be dual-enrolled in RPM and CCM programs. Patients benefit from more holistic care and healthcare organizations maximize their reimbursement opportunities – to the tune of $113 per patient per month.
Not all remote patient monitoring software systems are built the same. We work with you to understand your unique needs and tailor a solution that works for you and your business.

This quick reference guide covers key information on remote patient monitoring CPT codes, 2026 reimbursement rates, and billing workflows.
This on-demand webinar covers how Medicare's 2026 physician fee schedule final rule could impact remote care management programs.
This guide offers essential information and everything you need to know about identifying eligible RPM patients and completing the initiating visit.